HOME > Diabetes mellitus as a risk factor for dementia
Diabetes mellitus as a risk factor for dementia : epidemiological, radiological, and pathological evidence
Several studies have suggested that subjects with diabetes mellitus are at an increased risk of developing dementia. The Hisayama Study has comfirmed the association of diabetes with dementia, especially Alzheimer’s disease (AD), using three different methods, namely (1) the epidemiological (prospective cohort) study, (2) the neuroradiological (MRI) study, and (3) the autopsy-based neuropathological study.
Epidemiological evidence: the prospective cohort study
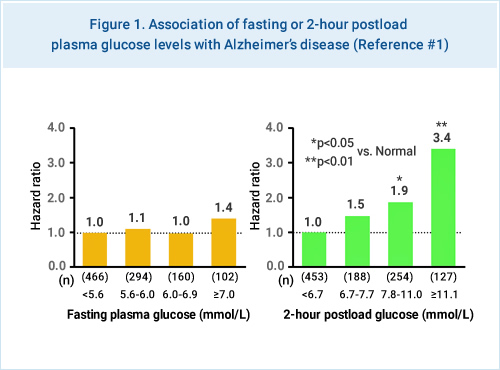
The elderly subjects in Hisayama aged 60 years or older with 75-g oral glucose tolerance test (OGTT) data were followed up from 1988 to 2003 to examined the association between fasting and 2-hour postload glucose levels and the risk of developing AD (Figure 1). Intriguingly, this study revealed that greater 2-hour postload plasma glucose levels, but not greater fasting plasma glucose levels, were linked to an increased risk of both AD and vascular dementia (VD) in an elderly Japanese population. These findings may suggest that hyperglycemia after glucose load is involved in the development of AD as well as VD.
Neuroradiological evidence: the MRI-based study
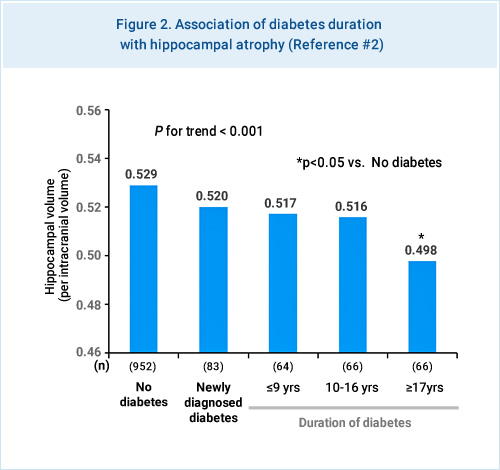
The morphological changes of AD occur in the hippocampus, amygdala, and medial temporal lobe in the early stages of the disease. The Hisayama Study investigated the association between diabetes and hippocampal atrophy in the elderly subjects aged 65 years or older, who underwent brain MRI scans in 2012. As a consequence, diabetic subjects had a significantly smaller hippocampal volume than non-diabetic subjects. Furthermore, longer duration of diabetes was significantly associated with smaller hippocampal volume (Figure 2).
Pathological evidence: the autopsy-based study
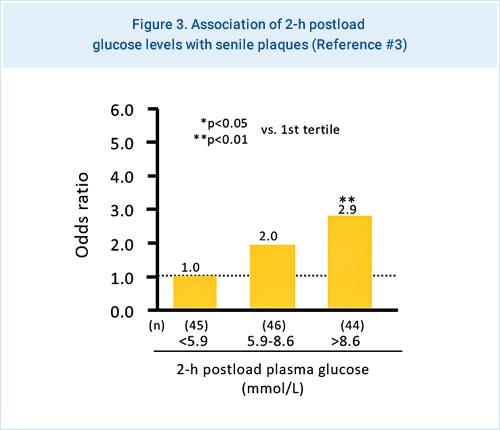
The autopsy-based pathological studies in Hisayama also showed the significant association between the diabetes-related factors and the neuropathology of AD. This study revealed that the risk of the presence of senile plaques increased significantly with elevating 2-hour postload glucose levels, fasting insulin, and HOMA-IR (a marker of insulin resistance), but not fasting plasma glucose level (Figure 3). This suggests that hyperinsulinemia and insulin resistance may be involved in the etiology of AD.
References
- 1. Ohara T, et al. Neurology 77: 1126-1134, 2011.
- 2. Hirabayashi N, et al. Diabetes Care 39: 1543-1549, 2016.
- 3. Matsuzaki T, et al. Neurology 75: 764-770, 2010.






